The Whole Health Model
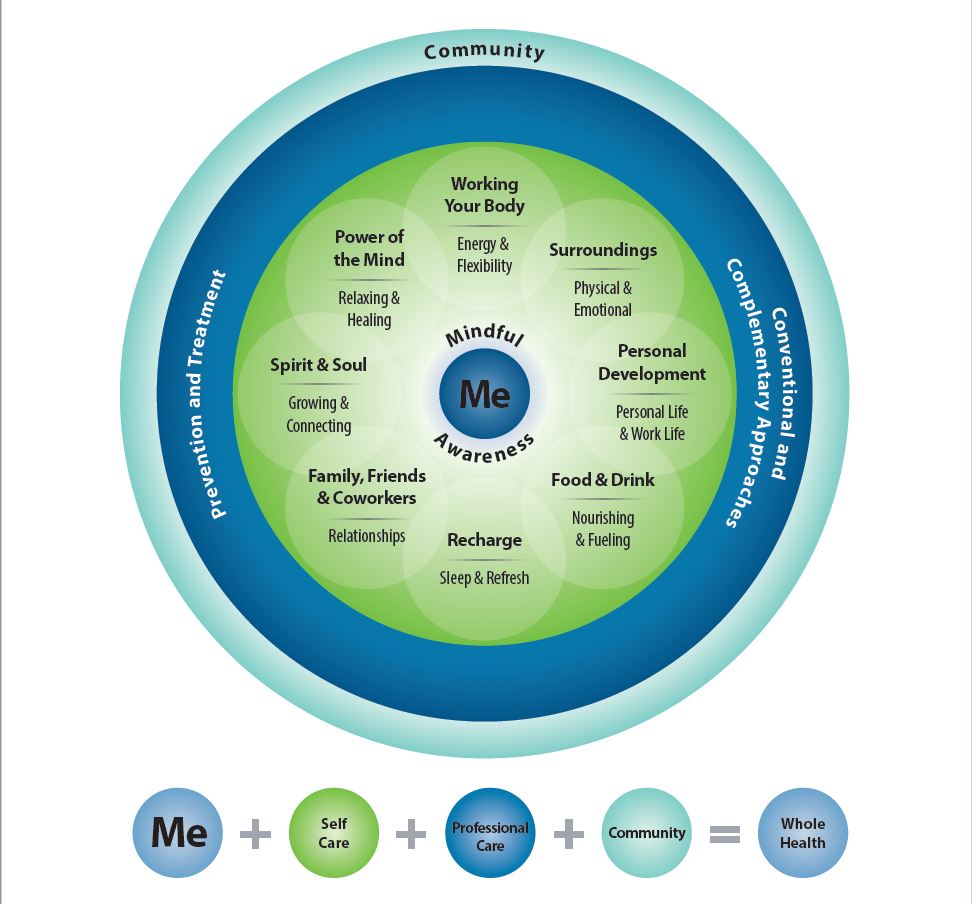
The Whole Health model for patient care is all encompassing—it is more than just treating a particular symptom or disease. Commonalities include:
- Recognizing the patient as a whole person, not just by diagnosis, illness, injury or disability,
- Examining the effects manifesting throughout the patient’s body, mind, and spirit to enhance the person’s life and total well-being.
- Placing the patient as an active partner at the center of all aspects of his or her health,
- Compiling a team to help the patient meet goals for overcoming health issues, as well as daily living, and future goals.
- Incorporating a range of conventional and complementary approaches, like mindfulness education to promote self-care and healing, and alternative therapies like yoga, acupuncture, massage, meditation, and biofeedback, among others.
- Emphasizing the importance of relationships and partnerships with a team of providers and community resources.
Physicians who practice using a whole health model have an expanded toolbox for care of the whole person—taking into consideration the patient’s current medical issues, plus past history and their life goals. This is particularly helpful for veterans who suffer with chronic pain and often experience comorbid mental and physical health issues such as addiction to opioids or other substances and Post Traumatic Stress Disorder (PTSD), among other diagnoses and symptoms. With Whole Health, the aim is to help veterans focus on life goals as they work to manage their chronic pain and other ailments. If patients are able to pinpoint why they want to be healthy, they are able to, with the help of a support team, develop a Personal Health Plan based on their goals, preferences, and needs. By doing so, they are empowered to carve out their own individual pathway toward well-being; one that incorporates self-care skills, complementary and integrative health, health coaching and support, clinical treatments, in/outpatient care, and health and disease management.
The Patient Experience with Whole Health
Although the model of Whole Health is relatively new, veterans who have been under the care of the VA’s Whole Health for Life model have shared their success stories. For one, veteran Alex Stallworth (Marine Corps 1985 – 1990) has been able to change his life under the Whole Health model. Now a trained Whole Health group facilitator, Stallworth shares a bit of his journey back to good health in a 2017 Veterans Health Administration (VHA) video1 (see video sidebar): “I could never have told my story if there were no ears to listen. Using the tools and techniques that the VA’s programs have taught me to be productive and constructive in my life. It has put me in the driver’s seat and empowered me to take control of my new beginning, my new life.”
This integrative method has also improved life for Larae Jackson (Airforce 1982 to 1992), who has been experiencing chronic pain related to Fibromyalgia since the mid ‘80s. “No one could figure out why,” she explains in a separate 2017 VHA video2 (see video sidebar). “For a long time, I felt alone. I felt that no one understood what I was going through. Moving in the direction that I am right now, I can walk on my treadmill, I can take my dogs to the park, I can sit through a whole movie, which I couldn’t do before, I can sleep, and I can have a social life. All has proven to be very important.”
Since veterans like Stallworth and Jackson and so many others like them, have benefited from this integrative approach to patient care, the VA is leading the approach to institute the Whole Health model for health care at VA sites across the country. Implementation of integrative medicine like the Whole Health model doesn’t have to be unique to the VA health system; the model can enhance and expand the patient care tool kits of all clinicians. When it comes to pain management, the broadened tool kits stemming from Whole Health may prove to offer patients better, more lasting solutions for their wellbeing.
The Whole Health Model for patient care encourages veterans develop a personal health plan to help their take charge of their health and well-being and to live their life to the fullest.
In the above video, both Veterans and VA providers talk about the process of using the whole health system approach in a clinical setting.
Instituting the Whole Health Model for Pain Management
- engage patients in practicing self-care, with a combination of provider and community support,
- use health IT infrastructure to enhance information distribution and community,
- offer practical guidance for care implementation, and
- focus on evidence-based integrative treatment approaches.3

William Becker, M.D., and Karen Seal, M.D. are co-PIs on a study meant to establish and implement a new Whole Health paradigm for chronic pain care, emphasizing non-pharmacological self-management of pain that reduces pain symptoms and improves overall functioning and quality of life in veterans. To learn more about their study as part of the PMC, click here.
Related Content
Integrative & Integrated Health Care for Managing Pain in Veterans
Karen Seal, MD, MPH, explains integrative and integrated healthcare, as well as the VA's Whole Health model, its components, and its benefits. Dr. Seal also...
Read MoreIntegrative Health: An Interview with Karen Seal, MD, MPH
Our PMC editor sat down with Dr. Seal to talk about alternative approaches to pain management, integrative medicine, the VA's Whole Health model for patient...
Read MoreAlternative Approaches to Pain Management
William Becker, MD, and Benjamin Oldfield, MD talk about their approach to non-opioid alternatives for effective pain management.
Read MoreFor more information on Whole Health, please see the following links:
Whole Health for Life
This page has a variety of Veteran whole health education handouts to support the Whole Health journey.
https://www.va.gov/patientcenteredcare/veteran-handouts/index.asp
Personal Health Inventory for Patients
Information on Whole Health and questionnaire for patients to complete.
http://projects.hsl.wisc.edu/SERVICE/sites/final/additional/mystory_phi.pdf
The Whole Health Library Website
General information about the Whole Health Library Website can be found on page 6:
http://projects.hsl.wisc.edu/SERVICE/
The Six Elements of Good Pain Care
As part of its Whole Health Model, the VA has established six points for safe and effective pain care.
/sixessentialelements
Footnotes
1. The Pathway to Whole Health (https://www.youtube.com/watch?time_continue=7&v=0nkO-3PA29c) Veterans Health Administration Published on July 12, 2017
2. Whole Health Approach to Clinical Care (https://www.youtube.com/watch?v=wrvHS8oMSWM) Veterans Health Administration Published on Sep 14, 2017
3. “Implementation of a Pragmatic Trial of Whole Health Team vs. Primary Care Group Education to Promote Non-Pharmacological Strategies to Improve Pain, Functioning and Quality of Life in Veterans”
- Grant # 1 UG 3AT009765-01.
- Funder: Northern California Institute for Research and Education (NCIRE).
- Institutes Providing Oversight:
- National Center for Complementary and Integrative Health (NCCIH);
- Eunice Kennedy Shriver National Institute of Child Health and Human Development (NICHD);\
- National Center for Medical Rehabilitation Research (NCMRR)
4. “Pain and Opioid Management in Veterans: Evidence, Lessons Learned, and Future Directions in the Use of Collaborative and Integrated Care Approaches.
- NIH Videocasting,
- Monday, April 10, 2017
- Link to Video




